-
-
- Council Members
- Role of Council Members
- Council meetings
- Council elections
- Previous election results
- Dr Louise Allum
- Dr Sam Bescoby
- Dr Andrew Clemence
- Dr Tshidi Gardiner
- Dr Reginald Godwin
- Paddy Gordon
- Dr Danielle Greenberg
- Dr Gerard Henry
- Dr Richard Hillman
- Dr Benjamin Kennedy
- Dr Tom Lonsdale
- Dr Darren Partridge
- Martin Peaty
- Alison Price
- Dr Peter Robinson
- Dr Jennifer Simmons
- Dr Sadie Spencer
- Dr Mary Thomas
- William Wilkinson
- Dr Lara Wilson
- Past-Presidents
-
- Advancement of the Professions Committee
- Standards Committee
- Audit and Risk Committee
- Education Committee
- Disciplinary Committee
- Charter Case Committee
- Preliminary Investigation Committee and Disciplinary Committee Liaison Committee
- Registration Committee
- Preliminary Investigation Committee
- Paper classification: some definitions
-
-
-
-
-
- About extra-mural studies (EMS)
- EMS requirements
- Information for vet students
- Information for EMS providers
- Information for vet schools
- Temporary EMS requirements
- Practice by students - regulations
- Health and safety on EMS placements
- EMS contacts and further guidance
- Extra-mural studies fit for the future
-
-
- Code of Professional Conduct for Veterinary Surgeons
- Code of Professional Conduct for Veterinary Nurses
- Contact the Advice Team
- XL Bully dog ban
- 'Under care' - guidance
- Advice on Schedule 3
- Controlled Drugs Guidance – A to Z
- Dealing with Difficult Situations webinar recordings
- FAQs – Common medicines pitfalls
- FAQs – Routine veterinary practice and clinical veterinary research
- FAQs – Advertising of practice names
- GDPR – RCVS information and Q&As
-
- Accrediting veterinary degrees
- Accrediting veterinary nursing qualifications
- Reasonable adjustments for student vets
- Reasonable adjustments for student veterinary nurses
- Health and disability in veterinary nurse education and training
- Reasonable adjustments for students and the UK disability discrimination legislation
- Educational assessment of veterinary nurses
- Roles of key stakeholders in the application of reasonable adjustments
- Examples of reasonable adjustments for vet nurse students
- External review of the RCVS by ENQA
- Requirements for remote and online student assessments
Practical case studies on communication and consent in clinical practice
In January 2018 the RCVS updated its guidance on communication and consent with more advice on discussing informed consent with clients and who is responsible for gaining consent.
The Codes of Professional Conduct for both veterinary surgeons and veterinary nurses stress the need for effective communication with clients and ensuring that informed consent is obtained and documented before treatments or procedures are carried out.
At its January meeting our Standards Committee approved changes to chapter 11 (‘Communication and consent’) of the supporting guidance to the Codes to provide further advice to the professions on matters that should be discussed with clients to ensure informed consent is gained, provide clarification on who can gain consent for a procedure and give some additional guidance on consent forms.
We have now published a series of case studies highlighting some of the issues commonly encountered in practice around gaining sufficient levels of consent for procedures, with learning points from the College about how the process could have been improved and references to the recent updates we have made to the guidance.
Case study 1: No consent teeth removal
This morning, Dr Mosse saw a new client, Sara. Sara explained that she had noticed that the mouth of George, her Labrador, smelt bad. After examining George, Dr Mosse explained that his teeth were thick with tartar and she would like to do a “dental procedure” on George. Sara asked if George would need any teeth removed. Dr Mosse reassured Sara that they would “let her know” if this was the case.
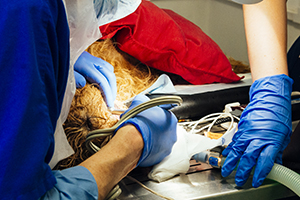 Sara signed a consent form for a clean and polish of the teeth, which included consent for ‘any other dental procedure as necessary in the best interests of the animal’, and left George at the practice for his surgery.
Sara signed a consent form for a clean and polish of the teeth, which included consent for ‘any other dental procedure as necessary in the best interests of the animal’, and left George at the practice for his surgery.
When Sara came to collect George in the afternoon, she was surprised and upset to hear that nine of George’s teeth were removed because they were loose and/or damaged.
Sara considered that the removal of nine teeth should have been discussed with her prior to it being done. Sara had told the practice that she would be near her phone all day if they needed to call for any reason, and the practice did not attempt to call.
Dr Mosse told Sara that the consent form that she had signed had given permission for the practice to perform other dental procedures, and that this could include teeth removal. Dr Mosse also claimed that she had talked through the benefits and risks of teeth removal when they agreed on an estimated cost. At the time of the surgery, Dr Mosse was under the impression that she had obtained informed consent from Sara for the removal of teeth.
Sara was not satisfied with this explanation, as, not only had the practice not asked for consent to remove teeth, but they had not even tried to obtain consent. Sara had interpreted the catch-all term on her consent form, which referred to consent for ‘any other dental procedure as necessary in the best interests of the animal’, to only apply in an emergency. As the removal of George’s teeth was not performed because of emergency circumstances, Sara considered that she had not provided consent.
Learning points
Under the Code of Professional Conduct for Veterinary Surgeons, ‘2.4 Veterinary surgeons must communicate effectively with clients… and ensure informed consent is obtained before treatments or procedures are carried out’.
Although there are caveats to this, such as not needing to obtain consent because the delay caused by doing so would adversely affect the animal’s welfare, this is unlikely to apply in this situation. In this case, no steps were taken to gain the additional consent for teeth removal as Sara was not contacted while George was under anaesthesia. There has been a clear miscommunication, as Sara had interpreted the situation differently to Dr Mosse.
Dental procedures are hard to predict, but this is not always well communicated to the client. Dr Mosse should have made it clear that, should the removal of teeth be required, that this would be performed as well as the scale and polish.
Good communication is vital prior to the procedure to ensure that the client is aware of what “dental treatment” entails, and the consent form should cover the likely range of both extractions and costs.
Chapter 11 of the supporting guidance to the Code advises that, where the outcome of the procedure is uncertain, this should be explained to the client, and the client should be made aware that they need to be available on the phone.
Alternatively, some veterinary surgeons may prefer to have agreed that after performing the initial assessment under anaesthetic that they will then contact the owner by phone, having previously warned them that this will be necessary, to discuss the further treatment required and an estimate of costs.
This is in line with paragraphs 11.2(h) and 11.18 of Chapter 11 to the Code:
11.2 […]
The following matters should be considered during the discussion with the client to ensure informed consent:
[…]
h. Ensuring, where possible, that consent can be obtained from the client for any deviations from the treatment plan (including costs), therefore where possible ensuring that the practice has the client’s emergency contact details and that these are up to date.
11.18 Provision should be made for uncertain or unexpected outcomes (e.g. in relation to dental procedures). Clients should be asked to provide contact telephone numbers to ensure discussions can take place at short notice. Provision for the veterinary surgeon or veterinary nurse to act without the client’s consent if necessary in the interests of the animal should also be considered.
Case study 2: Full range of options not given
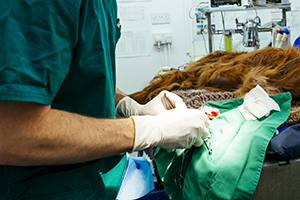 Buster, an Alaskan Malamute, was diagnosed with an osteosarcoma on his leg. His vet, Mrs Platell, knowing that Buster’s owner Ralph had struggled to pay for treatment in the past, suggested amputation of the leg, to which Ralph agreed. Ralph signed the consent form on the same day, and the surgery was performed the following week.
Buster, an Alaskan Malamute, was diagnosed with an osteosarcoma on his leg. His vet, Mrs Platell, knowing that Buster’s owner Ralph had struggled to pay for treatment in the past, suggested amputation of the leg, to which Ralph agreed. Ralph signed the consent form on the same day, and the surgery was performed the following week.
Buster recovered without incident, but when Ralph’s next-door neighbour saw Buster on three legs, he asked what had happened. When Ralph explained, the neighbour recalled a previous dog she had herself owned, which had had the same sort of tumour. Her vet at the time had discussed options including limb-sparing surgery, radiation for palliation or treatment, and chemotherapy.
The neighbour’s vet had also explained that, whatever treatment protocol is used for osteosarcomas, there is a high likelihood that they have already spread by the time of diagnosis. Consequently she had chosen to have her dog euthanased when the pain became uncontrollable.
Ralph called the practice immediately – he asked why he was not told of the other options, and why it was not explained that the cancer may have spread? Ralph said that knowing this would have changed his decision to amputate. He may instead have chosen to euthanase Buster, and he feels that he was not given the chance to make an informed decision about his dog’s treatment.
Learning points
In order for a client to give informed consent for treatment or procedures to be undertaken on their animal, they should have had the opportunity to consider a range of reasonable treatment options (paragraph 11.2 of the supporting guidance to the Code), not just the option that the veterinary surgeon considers to be the best in this case (11.2(g)).
Ralph should have also been informed of the potential benefits, risks, and likely outcomes of each treatment option (11.2(a) and (b)), including the mortality rate for the diagnosis.
As the surgery was not an emergency, Ralph should also have been given the chance to consider the options, and ask any questions. The opportunity to have a consultation with the vet to discuss these options may be useful, and euthanasia should always be presented as a treatment option where quality of life is affected (11.2):
11.2 Informed consent, which is an essential part of any contract, can only be given by a client who has had the opportunity to consider a range of reasonable treatment options (including euthanasia), with associated fee estimates, and had the significance and main risks explained to them. For non-urgent procedures, the consent discussion should take place in advance of the day of the treatment/procedure where possible. The client’s consent to treatment should be obtained unless delay would adversely affect the animal's welfare.
Case study 3: Cat castrated without consent
 Lucy phoned a local charity seeking veterinary treatment for one of the semi-feral stray cats she had been feeding in her back garden. She noticed that one of the cats, nicknamed Ginger, had developed a swollen face. Lucy believed that the cat had been owned by neighbours who had moved away, and she had been feeding it ever since.
Lucy phoned a local charity seeking veterinary treatment for one of the semi-feral stray cats she had been feeding in her back garden. She noticed that one of the cats, nicknamed Ginger, had developed a swollen face. Lucy believed that the cat had been owned by neighbours who had moved away, and she had been feeding it ever since.
The charity advised that they could arrange treatment for the cat, and agreed to pick the cat up and take it to the veterinary practice due to Lucy’s concerns about handling it. No written consent form was signed, and Lucy did not attend the practice.
Under anaesthetic, the swelling was found to be a large abscess, almost certainly caused by fighting. The charity had a policy of neutering stray cats. As Ginger was unneutered, he was castrated under the same anaesthetic, in accordance with the policy and considered in the cat’s best interest. The charity was billed for the procedure.
The charity collected Ginger and returned him to Lucy, who was happy to keep feeding him as a semi-feral, “community cat”. Lucy was not happy when she found out about the castration but was placated when it was explained how this would prevent similar problems in the future. However, a few days later, a neighbour of Lucy’s came to the practice to complain that they also fed Ginger and considered themselves to be his owner.
They were upset he had been neutered without their consent. Dr Tomassi explained that he had followed the charity’s standard procedure, which was for all stray cats treated by it to be neutered.
Learning points
Before carrying out any treatment or procedure, veterinary surgeons and veterinary nurses must obtain informed consent, as required by section 2.4 of the Code of Professional Conduct for Veterinary Surgeons.
Where the client is not the registered owner, care should be taken that the person giving consent has the authority to do so. It is important to be clear on who the client is, especially when dealing with stray cats, where ownership is often unclear.
In this case, the charity is the client, and it is sensible to ensure that the charity has explained this to any finder/feeder. If the finder/feeder wants to be dealt with as the client then they should be made aware of their responsibility under the Animal Welfare Acts to ensure that the animal’s welfare needs are met.
Ideally, the charity should have taken further reasonable steps to locate an owner, for example, by putting up posters, using lost and found websites and/or the practice’s website or social media pages. In general charities will wait a minimum of seven days before undertaking significant, non-emergency procedures such as neutering.
However, in cases where the history suggests ownership is unlikely and welfare is likely to be significantly enhanced by performing the procedure, such as trap/neuter/release of feral colonies, or neutering of semi-feral cats, the vet should keep good notes of their decision-making process but should not be unduly concerned about performing these procedures prior to seven days, if it is clearly in the best interest of the animal.
To meet the standards for ‘General Practice’ under the RCVS Practice Standards Scheme, a signed consent form should be obtained for all procedures, and when an animal is admitted to the care of a veterinary surgeon. A representative of the charity should sign this.
It is not sufficient to rely on a practice policy. If it is not practical for the treating vet to obtain the client’s consent themselves, they can delegate this responsibility, but only to a suitably trained person who has sufficient knowledge of the proposed procedure or treatment, and who understands the risks involved.
This is stated in new paragraph 11.3 of Chapter 11 of the RCVS supporting guidance:
11.3 Ordinarily it is expected that the veterinary surgeon undertaking a procedure or providing treatment is responsible for discussing this with the client and obtaining the client’s consent. If this is not practical, the veterinary surgeon can delegate the responsibility to someone else, provided the veterinary surgeon is satisfied that the person they delegate to:
a. Is suitably trained, and
b. Has sufficient knowledge of the proposed procedure or treatment, and understands the risks involved.
Case study 4: Euthanasia without consent
 Carlos’ elderly dog, a Corgi named Barney, had stopped eating and was off-colour. Carlos needed to go to work, but called his usual veterinary practice to ask for a vet to visit his house during the day to attend to Barney, as his sister would be there.
Carlos’ elderly dog, a Corgi named Barney, had stopped eating and was off-colour. Carlos needed to go to work, but called his usual veterinary practice to ask for a vet to visit his house during the day to attend to Barney, as his sister would be there.
Later that day a veterinary surgeon from the practice, Dr Preis, went to Carlos’ house to see Barney. Dr Preis had seen Barney at the practice about two months before, and had discussed Barney’s numerous health conditions, and the possibility that he may need to be euthanased in the near future.
After examining Barney, Dr Preis explained to Carlos’ sister that there were few treatment options available, and given the discomfort Barney appeared to be in, in her view euthanasia would be the best option. Carlos’ sister tried to call her brother but could not get through.
As Carlos could not be contacted, Dr Preis decided to proceed with euthanasia. Dr Preis later spoke to Carlos and told him that Barney had to be euthanased. Dr Preis explained that she had not obtained his consent first as she was unable to contact him, and in her opinion, Barney’s condition meant he should be euthanased without delay. She apologised that he had not had a chance to say goodbye.
Learning points
Veterinary surgeons and nurses must obtain informed consent, as required by section 2.4 of the Code of Professional Conduct for Veterinary Surgeons, unless delay would adversely affect the animal’s welfare.
The euthanasia procedure should not have taken place until Dr Preis had discussed it with Carlos and obtained his consent, unless in Dr Preis’s opinion Barney’s condition was such that he should in his own interests have been euthanised without delay.
Chapter 8 of the RCVS supporting guidance on euthanasia states, at paragraph 8.10, that a veterinary surgeon may need to act without the owner’s consent, but generally there should be discussions with the owner before such a decision, which should also be endorsed by a veterinary surgeon not directly involved in the case.
Chapter 11 of the RCVS supporting guidance also states, at paragraph 11.3, that ordinarily the veterinary surgeon is responsible for discussing procedures with the client and obtaining the client’s consent. Accordingly, Dr Preis should have tried to contact Carlos herself to discuss euthanasia and seek his consent. She should not have relied on her past discussions with him.
A sample form of consent for euthanasia is available on the webpage for Chapter 11. (The standards for ‘General Practice’ under the RCVS Practice Standards Scheme, provide that signed consent forms are usually required for all procedures when an animal is admitted to the care of a veterinary surgeon, including for euthanasia. “Admitted” means where an animal is in the care of the vet and not in the owner’s presence, including when being seen at the owner’s premises).
Case study 5: Verbal consent
 Bob, a lop-eared rabbit, was brought into the practice to be neutered. Bob’s owner, Julie, told the vet, Dr Wald, that she was worried about the procedure because she’d never owned an animal before. Dr Wald thoroughly explained the reasons why neutering of rabbits can be beneficial, but also stated that there are certain risks, as with any surgery.
Bob, a lop-eared rabbit, was brought into the practice to be neutered. Bob’s owner, Julie, told the vet, Dr Wald, that she was worried about the procedure because she’d never owned an animal before. Dr Wald thoroughly explained the reasons why neutering of rabbits can be beneficial, but also stated that there are certain risks, as with any surgery.
Julie and Dr Wald discussed the fee estimates, other routine procedures which may be undertaken (ie nail clipping and teeth cleaning, if needed), and then Dr Wald made sure that the practice held up-to-date contact details for Julie to make sure she could be contacted if needed. Dr Wald noted Julie’s verbal informed consent on the clinical records, and took Bob to be anaesthetised.
The surgery went well and Bob was expected to make a full recovery. However, when Julie went to collect Bob, she was surprised to see that Bob’s nails had been clipped, and one of the nails looked as if it had been bleeding. Dr Wald explained that, as part of the other routine procedures performed during surgery, Bob’s nails were clipped.
Unfortunately due to the dark colour of Bob’s nails it was difficult to establish where the ‘quick’ started, meaning that some of Bob’s sensitive tissues were damaged, leading to some bleeding. Dr Wald apologised and assured Julie that although unusual, the bleeding from the nail was very minor and would heal within a few days without further intervention.
Julie was very concerned as she did not believe that she had specifically consented to all of the procedures as she did not sign a consent form and she only had a verbal discussion with the vet. Julie decided to make a complaint to the practice manager and clinical director.
After reviewing the clinical records, the practice manager explained that, although she had not signed a consent form, Julie had provided verbal informed consent which was recorded on the clinical records and witnessed by Dr Wald and an animal nursing assistant. The practice manager offered a goodwill gesture to Julie, which she accepted.
Learning points
In routine circumstances, veterinary surgeons must ensure that informed consent is obtained from a client before treatment or procedures are carried out (Code of Professional Conduct 2.4). However, although a consent form can be a useful aid when explaining the procedure to clients (supporting guidance 11.6), there is no requirement for consent to be recorded on a consent form specifically.
Consent should always be recorded on the patient’s records however, and if this does not take place on a consent form then it should be noted on the clinical record that consent has been given or withheld (supporting guidance 13.1).
In this case, Dr Wald opted to not use a consent form, but was still able to ensure that the informed consent was evidenced on the clinical records. It was also useful that another member of staff was in the room to witness Julie’s consent.
Case study 6: No consent given for procedure
Robert was out for a walk with his partner when they spotted a horse that looked to be in distress. On closer inspection they could see that the horse had its head collar caught in a barbed wire fence which had cut the horse deeply along its neck. Robert called a local equine veterinary practice and Dr Streep agreed to come out and assess the horse.
The horse had been caught on public land, so it was unclear who the owner was. Dr Streep scanned the horse for a microchip, and, after contacting the microchip database, established that the horse was called Misty and was owned by Peter Jones. Dr Streep attempted to contact Peter using the phone number on the microchip, but the number was no longer in service.
Dr Streep’s concerns about Misty were growing as it was clear that she had been caught in the fence for a number of days, and, as well as her wounds, she was very hungry, dehydrated, and agitated. Dr Streep decided to proceed with treatment for Misty, even though she did not have informed consent from the owner. Dr Streep felt that Misty had already waited too long, and any further delay would adversely affect her welfare.
First aid and pain relief was administered to Misty, and Dr Streep enlisted the help of a local farmer to free Misty from the fence and bring her to the practice.
A few days later the practice received a phone call from Peter Jones, Misty’s owner. Once he realised that she was missing, Peter had been calling around local equine practices trying to find Misty. Dr Streep spoke to Peter and explained what had happened.
Peter was furious that treatment had been undertaken without his consent, and told Dr Streep that he would not be prepared to pay for the treatment. Peter also mentioned that he would be reporting Dr Streep to the RCVS as Dr Streep had not obtained consent.
Dr Streep explained to Peter that her first consideration when attending to animals is health and welfare, and that she is able to use her professional discretion to administer treatment without consent if the welfare of an animal is at risk.
Learning points
Although informed consent should be obtained before treatments or procedures are carried out (Code of Professional Conduct 2.4), there are exceptions to this obligation. The most commonly used exception is where the delay experienced in obtaining informed consent would adversely affect the health and welfare of the animal (supporting guidance 11.2), at which point a veterinary surgeon may choose to act without informed consent.
However, if the owner has not given informed consent for treatment, the vet needs to keep in mind that the owner may not be obliged to pay for that treatment. It may be that charity help is available in the area, although there is no guarantee of this and no charitable organisation has any statutory responsibility to cover costs.
Veterinary surgeons should accept that, in providing emergency treatment in these circumstances, they may not be paid, but this should not affect the decision as to whether to provide emergency treatment for the immediate relief of pain and suffering.
Case study 7: Hospitalisation - informed consent
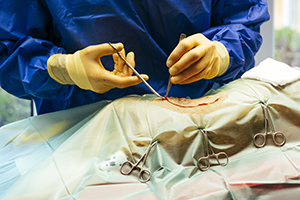 Nadia’s Staffordshire Bull Terrier, Freddy, had been vomiting for several days. As he has a tendency to eat rubbish out of the kitchen bin, she didn’t worry, until Freddy had not eaten for 36 hours. On examination at the veterinary clinic by Mr Moriarty, Freddy was found to be dehydrated, and a foreign body could be felt in his abdomen.
Nadia’s Staffordshire Bull Terrier, Freddy, had been vomiting for several days. As he has a tendency to eat rubbish out of the kitchen bin, she didn’t worry, until Freddy had not eaten for 36 hours. On examination at the veterinary clinic by Mr Moriarty, Freddy was found to be dehydrated, and a foreign body could be felt in his abdomen.
Mr Moriarty suggested that intravenous fluids be started, and surgery be undertaken later in the day. Unfortunately, the gut was damaged in the area where the foreign body was found, as there was a stone obstructing his small intestine. Mr Moriarty therefore decided to perform an enterectomy with end-to-end anastomosis.
Freddy was not well enough to be discharged so he was hospitalised overnight. He was checked at 10pm by a nurse, but when staff arrived at the surgery the next day, Freddy had died during the night.
Nadia questioned the attention that Freddy had received during the night. On being informed that staff performed intermittent checks but no-one was present in the building overnight, this added to her distress at losing Freddy, and she decided to make a complaint.
Learning points
Unless the practice is an RCVS-accredited hospital, there is no requirement to have a member of staff present overnight.
However, it is important that clients are informed of the level of supervision before they leave their animals. A professional judgment must be made about the level of care required by each patient, with consideration given to when the provision of care available at the practice is not sufficient for the animal’s condition, or acceptable to the owner. If the animal requires overnight supervision, there may be a need to refer the case to a nearby hospital or out-of-hours centre.
The costs of the out-of-hours options should be explained at the time of the initial discussion and as soon as possible once it appears that external out-of-hours care is advisable. It is recognised that the client may decline the recommended option due to cost limitations and the risks of this should be explained to them. It is advised that careful notes are made in this situation.
Chapter 2 of the supporting guidance to the Code of Professional Conduct states the following:
2.5 Veterinary surgeons and veterinary nurses should provide appropriate and adequate in-patient care.
2.6 Clients are entitled to have their animals housed in a comfortable environment, monitored and treated commensurate with the animal's condition, by persons with the requisite level of knowledge and expertise.
2.7 Before leaving an animal at a practice, the owner, keeper or carer should be made aware of the level of supervision that will be provided to the animal, particularly the level of supervision outside normal working hours. Different levels of care required arise in differing circumstances.
October 2018